Professional Documents
Culture Documents
Patient Monitoring System With SMS
Uploaded by
piyushji125Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Patient Monitoring System With SMS
Uploaded by
piyushji125Copyright:
Available Formats
MICROCONTROLLER
Abstract
BASED WITH
CARDIAC MONITORING SMS SERVICE
SYSYTEM
The project aims at developing a patient monitoring system. The system contains an ECG simulator to generate ECG waveform. The ECG simulator has control to vary heart rate as well as to generate different types of arrhythmias. The monitoring system keeps track of the heart rate activity. If there is any abnormality, it will send a SMS to a remote station to get the medical assistance. The ECG simulator is designed using an oscillator and pulse shaping circuit. The monitoring system contains an 8-bit ADC, 8-bit microcontroller and a GSM modem. The GSM modem is serially interfaced with the microcontroller. Standard AT command set is used to control GSM modem.
Block Diagram A typical ECG Circuit:
A ECG Simulator module will be developed which will provide the ECG waveform in its natural shape at the output.
The feedback from ECG module will pass through a missing pulse detector. The output of the missing pulse detector is high when the ECG continues. Any break in ECG will trigger the missing pulse detector to go high consequently triggering the microcontroller to generate a trigger for the emergency. Block Diagram:
LCD display
ECG Simulator
Missing pulse detection Circuit
Level Converter Microcontroller AT89C51
GSM MODEM Dialer
Major Components: AT89C51 Microcontroller GSM Modem (Serial Interface) IC555 Timer IC CD4521 CD4017 LM741 OPAMP IC7805 Voltage regulators IC 7815 Voltage regulator 16x2 Lampex LCD Rotary Switches BC547, BC557 NPN, PNP Transistors 1N4007 Diodes W10 Rectifier Resistance, Capacitors etc.
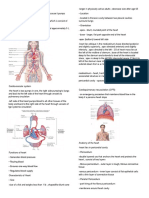
ECG Background William Einthoven developed the first electrocardiogram in 1903 using a crude galvanometer. Technology has advanced ECG measurement, but the principle remains the same. The electrocardiogram is the wave representation of the potential difference caused by heart activity. A grasp of the electrocardiogram has to be gained for two reasons: 1. An understanding of the wave forms the basis for the design of the electronic circuit to measure it; and 2. An understanding allows the concept of what an ECG is, and how its deviation enables analysis of health. The potential difference is created by the flux of ions in cells, a typical cell with Sodium and Potassium ions as shown in figure.
When the heart pumps, the cell wall offers greater permeability and an excess of sodium is able to flow inside the cell. When the sodium flows into the cell there is no longer a negative potential with respect to the outside. This is known as depolarisation. Eventually after the excitation passes, the cell repolarises, returning the potential to a negative one.
The standard for diagnostic ECG is twelve leads, however in the case of more portable, easy to use ECG one lead (usually Lead II) can be used. Lead II can diagnose the more common diseases like arrhythmias. Cells are originally polarised such that the potential inside each cell is negative with respect to the outside. Depolarisation occurs first, making the outside of the cell negative with respect to the inside. This imbalance causes an ionic current to flow, and the Left Arm to register a positive with respect to the right arm. This is known as the Pwave. The depolarisation then passes to the atrioventricular node. It is still relatively negative to the left ventricle causing a current and positive voltage from the left to right arms. This is the R-wave. The T wave is a representation of the repolarisation of the depolarised cells. Physicians can diagnose a persons health by reading these waves. From a signal processing perspective, the potential difference between left and right arms is typically 1-3mV and the frequency of the ECG signal lies between .02 and 150Hz. The quality of an ECG sensor could be categorised by its bandwidth. Usually sensors designed for the end of the market that this device was designed for only measure frequencies of up to 30Hz. If specifications for ECG emergency care were to be met, the frequency measured should extend to 1kHz. The problem with larger spectrums is that a proportional amount of noise must be battled with the frequencies that are measured. Glossary
ARRHYTHMIA: an abnormal rhythm of the heart beat. ASYSTOLE: a failure of the heart to beat or contract at a time when it should have. ATRIA: the top or collecting chambers of the heart. There are two of these, the right atrium and the left atrium. AV NODE: or atrioventricular node is a special conduction centre in the heart. It is located between the two lower chambers (ventricles) of the heart and receives the electrical impulse from the upper chambers (atria) of the heart and passes it downward into the lower chambers (ventricles). BLOOD PRESSURE: the pressure of the blood against the walls of the blood vessels. The term usually refers to arterial blood pressure. It is determined by the force of the heart beat, the resistance to the flow of blood in the arteries, the elasticity of the vessel walls, and the
bloods thickness. The blood pressure is expressed as one number over another, i.e., 120/80. The first number represents the systolic pressure and the second, the diastolic pressure. Both are recorded in millimetres of mercury. Strenuous physical activity, excitement, nervous tension, or fright raise the systolic pressure. BRADYCARDIA: a slow heart rate, generally under 50 beats per minute. BUNDLE BRANCH BLOCK: a blockage of one of the specialised conducting pathways within the lower chambers of the heart. BUNDLE OF HIS: also called common bundle or AV bundle. A bundle of specialised muscle fibres which conducts impulses from the AV node to the lower chambers of the heart. Named after Wilhelm His, a German medical scientist. CAPTURE: when a pacemaker impulse or discharge succeeds in causing the ventricles of the heart to beat or contract. CARDIAC OUTPUT: the amount of blood pumped by the heart per minute. CATHETERIZATION: in cardiology, the process of examining the heart by means of introducing a thin tube (catheter) into a vein or artery and passing it into the heart. The pacemaker lead inserted through the vein for pacing is a type of catheter. CIRCUITRY: the electrical portion of your pacemaker designed to pace the heart at a pre-established rate, and with a demand pacemaker, to sense your own underlying rhythm. CORONARY ARTERIES: the arteries that supply blood to the heart muscle itself. CARDIAC INSUFFICIENCY: inability of the heart to pump adequately. Causes shortness of breath, fluid retention, etc. DEMAND: a type of pacemaker that fires only when necessary; i.e., when the hearts own intrinsic rate becomes slower than the rate at which the pacemaker is programmed to operate. DEPOLARIZATION: electrical activity spreading through the heart, causing it to contract or beat.
DIASTOLE: relaxation of the heart between contractions. ECTOPIC: electrical stimulation of cardiac contractions beginning at a point other than the sinoatrial (SA) node. ELECTROCARDIOGRAM: often called EKG or ECG. It is a graphic record of the electric currents produced by the heart. ELECTRODE: the wire connecting the pacemaker (pulse generator) to the heart. It is responsible for carrying the electrical discharge to the heart and the sensed electrical activity of the heart back to the pacemaker. ENDOCARDIAL: refers to the inside layer of the heart. An endocardial electrode is one that is inserted via a vein, and the tip contacts the internal surface of the heart. EPICARDIAL: the outer layer of the heart. An epicardial electrode is one that is attached directly to the hearts outer surface. FIBRILLATION: rapid uncoordinated contractions of the heart muscle occurring when the individual muscle fibres take up independent irregular contractions. FIBROSIS: scarring of the heart or other organs of the body. Within the electrical portion of the heart this scarring may cause heart block or other rhythm disturbances. HEART BLOCK: a condition where the transmission of electrical discharges from the upper chambers of the heart to the lower chambers are partially or completely blocked, resulting in the chambers NOT working in a synchronised way. HYPERTENSION: an unstable or persistent elevation of blood pressure above the normal range. May eventually lead to an enlarged heart and kidney damage. HERMETIC SEAL: a process where the battery and circuitry of the pulse generator are sealed within a metal container that cannot be penetrated by body fluids. INTRINSIC RATE: patients own natural heart rate.
MYOCARDIAL INFARCTION: the damage or death of areas of the heart muscle (myocardium) resulting from a reduction in the blood supply reaching that area. NITROGLYCERIN: a medication used to relax the muscles in the blood vessels. Often used to relieve attacks of angina pectoris and spasm of coronary arteries. It is vasodilator. PACE: a condition in which a heart beat is initiated by a pacemaker. PAC: premature atrial contraction, a heart beat which has originated early in the upper chambers of the heart (atria). It is considered ectopic since it is not in the usual conduction pathway. PROGRAMMABLE PACEMAKER: a type of pacemaker which can be adjusted from the outside of the body using a specific instrument (programmer). The programmer can be used to vary the rate of pacing as well as the electrical output of the pacemaker. This does NOT require surgery. PULSE: a rhythm in the arteries caused by the contractions of the heart. PULSE GENERATOR: referring to the entire pacemaker; that is the circuitry and batteries together, which produce the periodic electrical impulse to the heart. PURKINJE FIBRES: specialised muscular fibres forming a network in the walls of the hearts lower chambers. Believed to be involved in conducting electrical impulses to the muscular walls of the ventricles. These impulses are responsible for the contractions of the ventricles. PVC: premature ventricular contraction. Similar to PAC but occurring within the lower chambers of the heart. RATE RESPONSE: a function that allows the pacemaker to increase the heart rate during exercise. REED SWITCH: a component of the circuitry of a demand pacemaker that is activated by placing a magnet over the unit. This causes a demand pacemaker to become a fixed-rate unit by bypassing the sensing circuitry. RHYTHM: a regular and repetitive recurrence of a beat.
SA NODE: sinoatrial node, the special nerve centre in the upper right chamber of the heart that in most instances initiates each beat. SENSE: the ability of a pacemaker to recognise the electrical impulse of a heart beat. SEPTUM: a thick muscular wall dividing the heart into right and left. SINUS RHYTHM: a normal type of rhythm initiated from the upper chambers of the heart with the electrical impulse passing normally into the lower chambers. STIMULUS: an electrical discharge by the pacemaker to the heart. STOKES / ADAMS ATTACKS: fainting spells associated with a temporary lack of perfusion of the blood to the brain generally associated with complete heart block. SYSTOLE: the contraction of the heart which forces blood through the arteries. SYNCOPE: fainting. TACHYCARDIA: a rapid heart rate usually over 120 beats per minute. THRESHOLD: the lowest amount of electrical energy from a pacemaker stimulus necessary to cause the heart to contract. TITANIUM: a type of metal used to make the outer case of the pacemaker. TRANSVENOUS: a type of electrode which is generally endocardial. It is inserted through a vein and passed to the heart, with the tip of the electrode placed in the endocardiumin. TRANSTHORACIC SURGERY: when an opening is made between the ribs so that epicardial electrodes can be sewn directly to the outer wall of the left ventricle. VENTRICLES: the lower chambers of the heart. There are two, the right and left ventricles. The right ventricle pumps blood to the lungs and the left ventricle pumps blood throughout the body.
Conclusion: The proposed project is a real demonstration of the working of a demand type pacemaker, which can take action in real time in the absence of feedback from heart. The pacemaker device is completely programmable which can provide varying output controllable by user. The project is proposed to be developed by using low cost components and thus it is economical and compact.
You might also like
- Active RF Id Reader DescriptionDocument2 pagesActive RF Id Reader Descriptionpiyushji125No ratings yet
- Electrical Component GuideDocument4 pagesElectrical Component Guidepiyushji125No ratings yet
- RelaysDocument15 pagesRelayspiyushji125No ratings yet
- Voice Recorder IcDocument43 pagesVoice Recorder Icpiyushji125No ratings yet
- Spy Robot New SynopsisDocument63 pagesSpy Robot New Synopsispiyushji125No ratings yet
- Performance Comparison and Analysis of DSDV and AODV For MANETDocument6 pagesPerformance Comparison and Analysis of DSDV and AODV For MANETHippihippyNo ratings yet
- Professional Charges For Workshop ConductionDocument1 pageProfessional Charges For Workshop Conductionpiyushji125No ratings yet
- Energy Efficient Approach For Converss: Routing Protocol For Wireless NetworksDocument4 pagesEnergy Efficient Approach For Converss: Routing Protocol For Wireless Networkspiyushji125No ratings yet
- Web Download Instruction - Only For WebsiteDocument2 pagesWeb Download Instruction - Only For Websitepiyushji125No ratings yet
- 1 Supply of Electronic Components As Per List Annexure IDocument10 pages1 Supply of Electronic Components As Per List Annexure Ipiyushji125No ratings yet
- Professional Charges For Workshop ConductionDocument1 pageProfessional Charges For Workshop Conductionpiyushji125No ratings yet
- Green CodeDocument10 pagesGreen Codepiyushji125No ratings yet
- Code PatDocument5 pagesCode Patpiyushji125No ratings yet
- SIM300 Application NoteDocument10 pagesSIM300 Application NoteDhananjaya NidubeNo ratings yet
- UnderwaterDocument3 pagesUnderwaterpiyushji125No ratings yet
- FDFDocument3 pagesFDFpiyushji125No ratings yet
- RF ID CardDocument5 pagesRF ID Cardpiyushji125100% (1)
- XbeeDocument33 pagesXbeepiyushji125No ratings yet
- 1 N N4007Document3 pages1 N N4007Trương Quốc HưngNo ratings yet
- V2I800183Document9 pagesV2I800183piyushji125No ratings yet
- Green CodeDocument10 pagesGreen Codepiyushji125No ratings yet
- Uc AT89s52: LCD Display KeypadDocument2 pagesUc AT89s52: LCD Display Keypadpiyushji125No ratings yet
- SMS based eNotice Board for CollegeDocument21 pagesSMS based eNotice Board for Collegepiyushji125No ratings yet
- MQ9Document3 pagesMQ9piyushji125No ratings yet
- Building Sensors and Motors For The Handy Board: Connector Wiring TechniqueDocument8 pagesBuilding Sensors and Motors For The Handy Board: Connector Wiring Techniquepiyushji125No ratings yet
- ArduinoDocument19 pagesArduinopiyushji125100% (2)
- DTMF DecoderDocument2 pagesDTMF DecoderShantanu ChakrabortyNo ratings yet
- Diploma B.E./B.Tech M.E./M.TechDocument1 pageDiploma B.E./B.Tech M.E./M.Techpiyushji125No ratings yet
- ClorDocument3 pagesClorpiyushji125No ratings yet
- Tutorial Eagle 5.11 enDocument70 pagesTutorial Eagle 5.11 enmaykepnhNo ratings yet
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5783)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (890)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (265)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (72)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Conceito de Pré Carga e Pós Carga em CardiologiaDocument9 pagesConceito de Pré Carga e Pós Carga em CardiologiarmesquitajrNo ratings yet
- Aritmije BoronDocument1 pageAritmije BoronKristijan GoldašićNo ratings yet
- Comparison of PSD of Normal and Abnormal ECGsDocument5 pagesComparison of PSD of Normal and Abnormal ECGsEduardoHernandezNo ratings yet
- Module-17 - CPR and AED PDFDocument28 pagesModule-17 - CPR and AED PDFJithinShankarNo ratings yet
- Cardiovascular Physiology: Cardiac Output, Blood Flow ControlsDocument33 pagesCardiovascular Physiology: Cardiac Output, Blood Flow ControlsLuiz Jorge MendonçaNo ratings yet
- Module 9 Lesson 4Document11 pagesModule 9 Lesson 4Faatoots FatsNo ratings yet
- DYSRHYTHMIASDocument9 pagesDYSRHYTHMIASgudobenNo ratings yet
- Contec Ms400 User Manual EngDocument28 pagesContec Ms400 User Manual EngLeonardo Quevedo100% (1)
- Atrial Fibrillation: Discussed by - DR Kunwar Sidharth SaurabhDocument45 pagesAtrial Fibrillation: Discussed by - DR Kunwar Sidharth SaurabhKunwar Sidharth SaurabhNo ratings yet
- Manejo Perioperatorio de MarcapasosDocument6 pagesManejo Perioperatorio de MarcapasosPao Sofía MoralesNo ratings yet
- Name Four Chambers: - Receive Blood From Systemic orDocument8 pagesName Four Chambers: - Receive Blood From Systemic orgabiNo ratings yet
- Practice Worksheets - Cardiac PhysiologyDocument5 pagesPractice Worksheets - Cardiac PhysiologyrickNo ratings yet
- Basicpacingconceptsppt2017-171221084227 2Document101 pagesBasicpacingconceptsppt2017-171221084227 2Bob RiouxNo ratings yet
- Heart Cardiovasc Chap12Document69 pagesHeart Cardiovasc Chap12Thea GornezNo ratings yet
- Basic EKG RefresherDocument210 pagesBasic EKG RefresherAaron D. Phoenix100% (6)
- Exam 1 Practice Questions Part 2Document109 pagesExam 1 Practice Questions Part 2NeoGellinNo ratings yet
- Emergency Drug Therapy 1ceuDocument7 pagesEmergency Drug Therapy 1ceuRN333No ratings yet
- Chapter 11-The Normal ElectrocardiogramDocument18 pagesChapter 11-The Normal Electrocardiogrammuna s100% (1)
- ECG-Naming The PRST Waves - (6!19!2012)Document7 pagesECG-Naming The PRST Waves - (6!19!2012)cornondaNo ratings yet
- Inotropes in PICU: Uses and Effects of Dopamine, Epinephrine, Dobutamine, Milrinone, Norepinephrine, and VasopressinDocument2 pagesInotropes in PICU: Uses and Effects of Dopamine, Epinephrine, Dobutamine, Milrinone, Norepinephrine, and VasopressinDijattxNo ratings yet
- SECTION 1 CHAPTER 1 Vital Signs MeasurementDocument15 pagesSECTION 1 CHAPTER 1 Vital Signs MeasurementRhea Andrea UyNo ratings yet
- Congestive Heart FailureDocument43 pagesCongestive Heart FailuresudersonNo ratings yet
- HeartDocument11 pagesHeartKei GauranoNo ratings yet
- Advances in Electrocardiograms - Clinical Applns. - R. Millis (Intech, 2011) WW PDFDocument340 pagesAdvances in Electrocardiograms - Clinical Applns. - R. Millis (Intech, 2011) WW PDFLisa BobulaNo ratings yet
- Blood Pressure Levels for Boys and Girls by Age and HeightDocument4 pagesBlood Pressure Levels for Boys and Girls by Age and HeightHo Yoke MeiNo ratings yet
- The Physiology of A Frog Heart With The Effects of Temperature, Neurotransmitters, and Electrical IsolationDocument17 pagesThe Physiology of A Frog Heart With The Effects of Temperature, Neurotransmitters, and Electrical IsolationAbir Hasan ShuvoNo ratings yet
- Unstable AnginaDocument11 pagesUnstable AnginaAdrian BoboceaNo ratings yet
- Heart Failure Nursing Care Plans - 15 Nursing Diagnosis - NurseslabsDocument13 pagesHeart Failure Nursing Care Plans - 15 Nursing Diagnosis - NurseslabsJOSHUA DICHOSONo ratings yet
- Exam1 100731100921 Phpapp02Document34 pagesExam1 100731100921 Phpapp02Yaj CruzadaNo ratings yet
- 20 Questions in CPRDocument5 pages20 Questions in CPRأبوأحمد الحكيم100% (1)