Professional Documents
Culture Documents
4 16 14 Vascular Disease and Respiratory Failure Small Group Cases (Compatibility Mode)
Uploaded by
lessank12Original Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
4 16 14 Vascular Disease and Respiratory Failure Small Group Cases (Compatibility Mode)
Uploaded by
lessank12Copyright:
Available Formats
4/14/2014
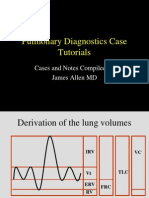
Vascular Disease And Respiratory Failure Case Tutorials
Cases and Notes Compiled by James Allen MD
Case #1
History: 20 yr old Caucasian woman with acute dyspnea, pleuritic chest pain, and hemoptysis PMH: recently started birth control pills SH: OSU student; non-smoker FH: father had phlebitis after hip surgery Exam: HR = 122, RR = 24, BP = 92/60, lungs clear to auscultation
Case #1: ABG
pH PCO2 PO2 HCO3 SaO2 7.50 25 55 21 90%
4/14/2014
Case #1: PFTs
FVC FEV1 FEV1/FVC TLC DLCO 3.27 liters 2.75 liters 92% 4.98 liters 100% 100% 100%
12.3 ml/min/mm 52%
Case #1: Chest X-ray
Case #1: Discussion
What is the differential diagnosis? How would you confirm the diagnosis? What are the likely contributing causes of this disease? How would you treat her? What would you advise her to do regarding future contraception?
4/14/2014
Pulmonary Embolus: Chest CT
4/14/2014
Pulmonary Embolus: Ventilation/Perfusion (V/Q) scan
Ventilation
Perfusion
Pulmonary Embolus: Pulmonary Angiogram
Pulmonary Embolus: Pathology
4/14/2014
Pulmonary Infarction: Pathology
Pulmonary Embolus: Pathology
Pulmonary Embolus
4/14/2014
Older Pulmonary Embolus
Very Old Pulmonary Embolus
Case #2: History
30 year old woman with progressive dyspnea over the past 9 months; she is now unable to carry out household chores and unable to walk 1 flight of stairs Past medical history: normal Social history: married with 2 children Family history: no cardiopulmonary disease
4/14/2014
Case #2: Physical Exam
Vital signs:
225 pounds HR 78 BP 130/79 RR 18
Lungs clear to auscultation 1/VI systolic murmur, loud pulmonic component of the second heart sound, elevated jugular venous pressure Mild pedal edema
Case #2: Chest x-ray
Case #2: Chest x-ray
29 cm 18 cm
4/14/2014
Case #2: PFTs
FVC FEV1 FEV1/FVC TLC Diffusing capacity 2.95 L 2.37 L 80% 4.97 L 16.5 (79%) (75%) (90%) (66%)
6 minute walk: SaO2 98% at rest and 91% while walking
Discussion Questions
What does her physical examination suggest? How do you interpret the chest x-ray? How do you interpret the PFTs? What is the significance of the 6 minute walk results? What additional studies would you order?
Case #2: Cardiac Echo
Normal left ventricle Dilated, hypokinetic right ventricle Dilated pulmonary arteries No evidence of intracardiac shunt
4/14/2014
Case #2: Right Heart Catheterization
Before iNO:
PA = 101/43 Mean PA = 65 PCWP = 7 CO = 4.7 CI = 2.3
After iNO:
PA = 88/42 Mean PA = 56 PCWP = 7 CO = 4.9 CI = 2.6
Discussion Questions:
What is the diagnosis? What is the prognosis? How would you treat her?
Case #3: History
45 year old caucasian man with shortness of breath worsening over the past 3 years. Past medical history: scleroderma Social history: disabled engineer; married with 2 children; non-smoker
4/14/2014
Case #3: Physical Exam
Vital signs:
HR RR BP 104 18 132/72
Lungs clear to auscultation Heart = tachycardic but regular; loud P2; elevated jugular venous pressure; II/VI systolic murmur at right sternal border
Case #3: Chest x-ray
Discussion Questions
What are the pulmonary complications of scleroderma? Which one is most likely in this case? What additional tests could you do to confirm your clinical suspicion? What physical examination findings support this diagnosis? What would a cardiac echo show?
10
4/14/2014
Case #3: Right Heart Cath
Pulmonary artery pressure = 97/41 (mean = 50) Pulmonary capillary wedge pressure = 8 Cardiac output = 3.6 Cardiac index = 1.8
Case #3: Pathology
Case #3: Pathology
11
4/14/2014
Discussion Questions
How would you treat him? Why is a pulmonary capillary wedge pressure important to measure when evaluating pulmonary hypertension?
Case #4
51 year old man with new onset seizures and status epilepticus Persistent seizures despite Dilantin, phenobarbital, and Propofol Intubated and started on pentobarbital drip for pentobarbital coma He developed pneumonia after 1 week that improved with antibiotics
Case #4 (continued)
After 2 weeks, he continues to have seizures when the pentobarbital is held. He remains comatose on a ventilator. On rounds, you note that he has developed hypoxemia resulting in an increase in his inhaled oxygen concentration from 30% to 100% On exam, he has new swelling of the right leg
12
4/14/2014
Case #4 (continued)
What is the most likely diagnosis? What test could you do to prove this diagnosis?
13
4/14/2014
Image courtesy of GE Healthcare; used with permission
Image courtesy of GE Healthcare; used with permission
Image courtesy of GE Healthcare; used with permission
14
4/14/2014
Image courtesy of GE Healthcare; used with permission
Case #4 (continued)
What is this patients risk factor(s) for this condition? What could have been done to prevent it? What other tests could have been used in the diagnosis of this condition?
Case #5
History: 44 yr old African American woman admitted with diverticulitis. 6 days after admission, she is febrile and dyspneic PMH: non-insulin dependent diabetes; prior MI SH: non-smoker FH: diabetes Exam (day 6): temp 102, RR = 32, HR = 136, BP = 74/52; severe respiratory distress; lungs clear to auscultation
15
4/14/2014
Case #5: ABGs (on 100% supplemental oxygen face mask)
pH PCO2 PO2 HCO3 SaO2 7.24 25 52 12 (anion gap = 22) 85%
Case #5: Chest X-rays
Admission
Hospital Day #6
Case #5: Chest CT
16
4/14/2014
Case #5: Additional Tests
Cardiac echo: LV ejection fraction = 42% Pulmonary artery catheter (Swan-Ganz): pulmonary capillary wedge pressure = 10 mm Hg Blood cultures: E. coli
Case #5: Discussion
What are the possible causes of her pulmonary infiltrates and hypoxemia? How do you know if this is acute respiratory distress syndrome (ARDS) vs. heart failure? How should she be managed immediately?
ARDS pathology
17
4/14/2014
Case #6: History
19 year old man with increasing confusion and morning headaches Past medical history: Duchennes muscular dystrophy; no surgery, no current medications Social history: disabled after high school Family history: first degree relatives healthy
Case #6: History
Review of systems: wheelchair bound; some difficulty swallowing; requires assistance with activities of daily living
Case #6: Physical Exam
Vital signs:
Afebrile RR = 16 HR = 102 BP = 100/68
Diffuse muscle atrophy Lungs clear to auscultation but both diaphragms elevated to percussion
18
4/14/2014
Case #6: Chest x-ray
Case #6: PFTs
FVC FEV1 FEV1/FVC TLC Diffusing capacity 1.76 L (52%) 1.48 L (56% 84% 3.54 L (60%) 24 (120%)
Case #6: ABG
pH PO2 PCO2 HCO3 SaO2 7.30 62 68 35 91%
19
4/14/2014
Discussion Questions
Is this hypercarbic or hypoxemic respiratory failure? What is the cause of his respiratory failure? What is the cause of his confusion? How would you treat him? What is the prognosis?
Case #7: History
60 year old woman with cough and increasing dyspnea for 2 weeks. Her family physician started oral steroids and antibiotics 4 days ago (for presumed exacerbation of COPD) with no benefit yet. For the past 24 hours, she has become much more short of breath Past medical history:
Illnesses: emphysema Surgery: cholecystectomy 10 years ago
Case #7: History
Medications:
Atrovent (inhaled bronchodilator) Serevent (inhaled bronchodilator) Prednisone 40 mg/day (oral steroid) Doxycycline (oral antibiotic)
Social history: 60 pack year smoker - still smokes; real estate agent; divorced
20
4/14/2014
Case #7: History
Family history: mother died of myocardial infarction; father died of stroke Review of systems: cough productive of yellow sputum; unable to climb one flight of stairs
Case #7: Physical Exam
Vital signs:
Afebrile RR = 32 HR = 112 BP = 134/80
Severe respiratory distress; only able to speak 2-3 words per breath Lungs - barely audible breath sounds; prolonged expiratory phase of respiration
Case #7: Chest x-ray
21
4/14/2014
Case #7: ABG
Room Air:
pH PO2 PCO2 HCO3 SaO2 7.18 52 74 28 85%
60% oxygen:
pH PO2 PCO2 HCO3 SaO2 7.12 72 80 29 92%
Discussion Questions
Is the main problem acute hypoxemic or hypercarbic respiratory failure? What is the cause of her respiratory failure? How would you treat her respiratory failure?
Case #7: Follow-up
After you successfully manage her in the hospital, her acute illness has resolved and she follows up in your office 2 months later Although her dyspnea has improved, she can only walk one flight of steps and is unable to return to work as a realtor because of limiting dyspnea when showing houses
22
4/14/2014
Case #7: Outpatient ABG
Room Air:
pH PO2 PCO2 HCO3 SaO2 7.38 52 42 25 87%
SaO2 while walking in the clinic hallway = 78%
Discussion Questions
Is her chronic respiratory failure hypercarbic or hypoxemic? How would you treat her?
23
You might also like
- Preoperative Evaluation GuideDocument49 pagesPreoperative Evaluation GuideGeeta KulkarniNo ratings yet
- USMLE Step 3 CCS NotesDocument20 pagesUSMLE Step 3 CCS Notesaustinhitz96% (25)
- Back to Basics: Critical Care Transport Certification ReviewFrom EverandBack to Basics: Critical Care Transport Certification ReviewNo ratings yet
- Information and Resources For Effective Self-Management of Problem Substance UseDocument52 pagesInformation and Resources For Effective Self-Management of Problem Substance Useedmidler100% (1)
- Suspecting Pulmonary Hypertension in The Dyspneic Patient: Who, When, and HowDocument92 pagesSuspecting Pulmonary Hypertension in The Dyspneic Patient: Who, When, and HowJonathan LongNo ratings yet
- COPD and Comorbidities Case StudyDocument66 pagesCOPD and Comorbidities Case StudyAzima Abdelrhaman100% (4)
- Graves DiseaseDocument7 pagesGraves DiseaseNader SmadiNo ratings yet
- Auricular Acupuncture: Prof - Dr.Murugeshbabu, M.SC, M.SC, M.PHIL, M.ACU, M.D, PH.DDocument74 pagesAuricular Acupuncture: Prof - Dr.Murugeshbabu, M.SC, M.SC, M.PHIL, M.ACU, M.D, PH.DMurugesh BabuNo ratings yet
- June 2014 Questions Returned From Candidates - Thank You: Long Case 1Document14 pagesJune 2014 Questions Returned From Candidates - Thank You: Long Case 1karan270No ratings yet
- Histology of The Cardiovascular System-3Document54 pagesHistology of The Cardiovascular System-3lessank12No ratings yet
- Post Op InstructionsDocument5 pagesPost Op InstructionsAmar Bhochhibhoya0% (1)
- Physical Examination in Cardiovascular Chinese MedicineFrom EverandPhysical Examination in Cardiovascular Chinese MedicineNo ratings yet
- Mock Papers for MRCPI, 3rd Edition: Four Mock Tests With 400 BOFsFrom EverandMock Papers for MRCPI, 3rd Edition: Four Mock Tests With 400 BOFsNo ratings yet
- Dental Caries IndexDocument35 pagesDental Caries Indexdr parveen bathla100% (1)
- Karapitiya OSCE 2017 With AnswersDocument34 pagesKarapitiya OSCE 2017 With Answersweerawarna fernandoNo ratings yet
- QSEN Simulation Template Post CABG PatientDocument8 pagesQSEN Simulation Template Post CABG PatientMissK2216No ratings yet
- CFPC SampsDocument39 pagesCFPC SampsSumer Chauhan100% (9)
- Wgu Pathophysiology Study Guide d236 Pathophysiology Exam Questions Completed With Correct AnswersDocument12 pagesWgu Pathophysiology Study Guide d236 Pathophysiology Exam Questions Completed With Correct Answersandrew kasaine100% (1)
- Case Studies On CoagulationDocument3 pagesCase Studies On CoagulationGerald John PazNo ratings yet
- MBChB Year 4 & 5 Past Papers + AnswersDocument170 pagesMBChB Year 4 & 5 Past Papers + AnswersHariharan NarendranNo ratings yet
- CHF Case StudyDocument38 pagesCHF Case StudyMelissa David100% (1)
- Nebulizing & Suctioning TechniquesDocument23 pagesNebulizing & Suctioning TechniquesRifky Octavio PNo ratings yet
- Clinical Case Report on Dengue FeverDocument16 pagesClinical Case Report on Dengue FeverAimanazrul ZainudinNo ratings yet
- Accident and Emergency Posting Case Write UpDocument8 pagesAccident and Emergency Posting Case Write UpAmbhi Gana0% (1)
- Nursing Care Plan-OBDocument20 pagesNursing Care Plan-OBPriscilla Paula Benavidez100% (3)
- NCLEX ExamDocument26 pagesNCLEX ExamNaufal Fadli AmzarNo ratings yet
- Ern MRCPCHDocument24 pagesErn MRCPCHPasTestBooksNo ratings yet
- Case Clerking MIDocument13 pagesCase Clerking MIKhairi Abd RahimNo ratings yet
- Cough, Dyspnoea: DR - Veena 2016 - 2017Document109 pagesCough, Dyspnoea: DR - Veena 2016 - 2017HanisahNo ratings yet
- Part 2: Patient History: Chief ComplaintDocument11 pagesPart 2: Patient History: Chief ComplaintDavid Lim Su Shen100% (2)
- Exam Orient-Focus HistoryDocument65 pagesExam Orient-Focus Historyyoune6No ratings yet
- Assess New Patient with UTI and DiabetesDocument11 pagesAssess New Patient with UTI and DiabetesNancy Cummings0% (1)
- Copy-A CASE OF ALTERED SENSORIUM - ALOKDocument37 pagesCopy-A CASE OF ALTERED SENSORIUM - ALOKAlok MohanNo ratings yet
- SGH How To Approach SBAsDocument49 pagesSGH How To Approach SBAsArnav RaiNo ratings yet
- Endocrine Case StudiesDocument36 pagesEndocrine Case StudiesaagarwalmdNo ratings yet
- HCV CasesDocument40 pagesHCV CasesEleni HagosNo ratings yet
- April 21st Recalls With Approaches and AMC Feedback Recollected From Several Posted MaterialsDocument6 pagesApril 21st Recalls With Approaches and AMC Feedback Recollected From Several Posted MaterialsqurbanNo ratings yet
- BPDDocument27 pagesBPDDana GeorgianaNo ratings yet
- Cardio Case StudentDocument5 pagesCardio Case StudentReynald Ddc ShiroNo ratings yet
- Diploma in Medical and Health Science Case ClerkingDocument9 pagesDiploma in Medical and Health Science Case ClerkingWan AmeeramirulzamanNo ratings yet
- Urine Case 2010-2Document9 pagesUrine Case 2010-2hendra_darmawan_4No ratings yet
- Discuss options with family - consider lung transplant evaluation vs palliative careDocument53 pagesDiscuss options with family - consider lung transplant evaluation vs palliative careHoa Cỏ ĐậuNo ratings yet
- Case PresDocument5 pagesCase PresJestoni GutierrezNo ratings yet
- C PulseDocument17 pagesC PulseJames SuarezNo ratings yet
- 0630 - Saturday - SEEK - GrossmanDocument101 pages0630 - Saturday - SEEK - Grossmantechang1No ratings yet
- IM Gastro Case1Document2 pagesIM Gastro Case1MaAngelicaElimancoNo ratings yet
- Physician Vignette-Answer Key 1 I-TECH Clinical Mentoring ToolkitDocument5 pagesPhysician Vignette-Answer Key 1 I-TECH Clinical Mentoring Toolkitnada adilahNo ratings yet
- 1.hess's TestDocument24 pages1.hess's TestRhomizal MazaliNo ratings yet
- Preoperative Preparation: Department Anesthesiology & Reanimation Medical Faculty Lampung UniversityDocument60 pagesPreoperative Preparation: Department Anesthesiology & Reanimation Medical Faculty Lampung UniversityDesty ArianiNo ratings yet
- Publishing Case Reports: 8 Tips for SuccessDocument48 pagesPublishing Case Reports: 8 Tips for Successsryh2012No ratings yet
- NCMB312 - : Bachelor of Science in Nursing: Communicable Disease NursingDocument7 pagesNCMB312 - : Bachelor of Science in Nursing: Communicable Disease NursingMichelle Gliselle Guinto MallareNo ratings yet
- Scenario Details: Scenario Title Chief Complaint Notes (Moulage, Equipment, Scene-Size Up Info, Etc.) ObjectivesDocument3 pagesScenario Details: Scenario Title Chief Complaint Notes (Moulage, Equipment, Scene-Size Up Info, Etc.) ObjectivesErwin RomeroNo ratings yet
- CVS Study Guide 2023Document28 pagesCVS Study Guide 2023Muhammad SulamanNo ratings yet
- Suggested Discharge SummaryDocument2 pagesSuggested Discharge SummaryJohnNo ratings yet
- Nursing Management of A Patient With: HyperthyroidismDocument31 pagesNursing Management of A Patient With: Hyperthyroidismember parkNo ratings yet
- ED Triage Prioritization: Understanding the Emergency Severity IndexDocument33 pagesED Triage Prioritization: Understanding the Emergency Severity IndexfadiNo ratings yet
- CC 4 Nov 2017 SeizureDocument44 pagesCC 4 Nov 2017 SeizurenisaNo ratings yet
- Overview of Hiccup Study DetailsDocument4 pagesOverview of Hiccup Study DetailsphreonburnNo ratings yet
- Ccc2012 HF WkshopDocument97 pagesCcc2012 HF WkshopHope EkwensiNo ratings yet
- Lapjag Bangsal IPD 22 OKTOBER DHFDocument57 pagesLapjag Bangsal IPD 22 OKTOBER DHFLeony Nerry SabatiniNo ratings yet
- CC 4 Nov 2017 SeizureDocument44 pagesCC 4 Nov 2017 SeizureLilik NatasubrataNo ratings yet
- Year 4 Formative Paper 3 2005Document10 pagesYear 4 Formative Paper 3 2005destroycheatingNo ratings yet
- Preoperative Preparation: Assessing Risk and Ensuring SafetyDocument60 pagesPreoperative Preparation: Assessing Risk and Ensuring SafetyDesty ArianiNo ratings yet
- Comprehensive History and Physical Note Subjective:: Breast ConcernsDocument3 pagesComprehensive History and Physical Note Subjective:: Breast ConcernsColton JohnNo ratings yet
- Neardrowning: Prehospital and Emergency Department ManagementDocument34 pagesNeardrowning: Prehospital and Emergency Department ManagementAyeNo ratings yet
- Special CirculationsDocument29 pagesSpecial Circulationslessank12100% (1)
- Regulation of Organ Blood Flow - PPT-2Document32 pagesRegulation of Organ Blood Flow - PPT-2lessank12No ratings yet
- Formation and Regulation of The Hemostatic Plug: Amy S. Gewirtz, MD Amy - Gewirtz@osumc - EduDocument62 pagesFormation and Regulation of The Hemostatic Plug: Amy S. Gewirtz, MD Amy - Gewirtz@osumc - Edulessank12No ratings yet
- 4 1 14 Histology of The Cardiovascular System Handout Baker 2Document7 pages4 1 14 Histology of The Cardiovascular System Handout Baker 2lessank12No ratings yet
- Cardiac Cycle: Heart Murmurs: Mary Beth Fontana MDDocument43 pagesCardiac Cycle: Heart Murmurs: Mary Beth Fontana MDlessank12No ratings yet
- 4 4 14 Cardiac Cycle and Heart Sounds Parts I II Fontana 3Document32 pages4 4 14 Cardiac Cycle and Heart Sounds Parts I II Fontana 3lessank12No ratings yet
- Cardiac Imaging Module 1A-2Document39 pagesCardiac Imaging Module 1A-2lessank12No ratings yet
- Pulmonary Diagnostics Case Tutorials: Cases and Notes Compiled by James Allen MDDocument46 pagesPulmonary Diagnostics Case Tutorials: Cases and Notes Compiled by James Allen MDlessank12No ratings yet
- Morphologic Compensatory Mechanisms in The Heart: Peter B. Baker, M.DDocument16 pagesMorphologic Compensatory Mechanisms in The Heart: Peter B. Baker, M.Dlessank12No ratings yet
- UNAIDS Core Epidemiology Slides enDocument11 pagesUNAIDS Core Epidemiology Slides enTabarcea VitaliNo ratings yet
- Starting Injectable RCN PDFDocument40 pagesStarting Injectable RCN PDFPhilip HartleyNo ratings yet
- The Lightning-Fast Quest For COVID Vaccines - and What It Means For Other DiseasesDocument3 pagesThe Lightning-Fast Quest For COVID Vaccines - and What It Means For Other DiseasesKathiravan M NNo ratings yet
- Anatomi Dan Fisiologi PerkemihanDocument89 pagesAnatomi Dan Fisiologi Perkemihannia djNo ratings yet
- Curriculum Vitae of Professor Francesco RiaDocument9 pagesCurriculum Vitae of Professor Francesco RianoncanimussurdisNo ratings yet
- Nellcor Puritan Bennett 740 VentilatorDocument2 pagesNellcor Puritan Bennett 740 VentilatorVictor daniel GraterolNo ratings yet
- Best Hospitals MethodologyDocument125 pagesBest Hospitals MethodologyAngeline YeoNo ratings yet
- What is GastroschisisDocument6 pagesWhat is GastroschisisAnonymous MWd5UOUuiyNo ratings yet
- HealthDocument6 pagesHealthAngel Bernal PinedaNo ratings yet
- Systemic in Ammatory Response Syndrome (SIRS) : Where Did It Come From and Is It Still Relevant Today?Document8 pagesSystemic in Ammatory Response Syndrome (SIRS) : Where Did It Come From and Is It Still Relevant Today?Jhanu JaguarNo ratings yet
- Introduction To Operation SuiteDocument12 pagesIntroduction To Operation Suitekamalab04No ratings yet
- Penicillin Drug StudyDocument2 pagesPenicillin Drug StudyEmagra AzilNo ratings yet
- Format HISTORY OF PATIENTDocument4 pagesFormat HISTORY OF PATIENTShiva CharakNo ratings yet
- Poster PresentationDocument1 pagePoster PresentationVency KatiraNo ratings yet
- Nursing Grand Rounds Reviewer PDFDocument17 pagesNursing Grand Rounds Reviewer PDFAlyssa Jade GolezNo ratings yet
- Nursing Care Plan#2kidneyDocument3 pagesNursing Care Plan#2kidneythubtendrolmaNo ratings yet
- AEBA QUESTIONS-WPS OfficeDocument2 pagesAEBA QUESTIONS-WPS OfficeMarj Castor LisondraNo ratings yet
- TTTTDocument26 pagesTTTTMoataz TrabehNo ratings yet
- DSM-IV Introduction: Understanding the Multiaxial Assessment SystemDocument3 pagesDSM-IV Introduction: Understanding the Multiaxial Assessment SystemRoci ArceNo ratings yet
- Free Journal List For PublicationDocument11 pagesFree Journal List For PublicationSyed Saad AliNo ratings yet
- Ultrasound-Guided Brachial Plexus BlockDocument7 pagesUltrasound-Guided Brachial Plexus BlockÇağdaş BaytarNo ratings yet
- Hip DislocationDocument4 pagesHip DislocationcrunkestNo ratings yet
- Name of DrugDocument6 pagesName of DrugKathleen ColinioNo ratings yet
- Microbiology of Clostridium Tetani and Wound ClassificationDocument3 pagesMicrobiology of Clostridium Tetani and Wound ClassificationAZIZAH ARDINALNo ratings yet