Professional Documents
Culture Documents
Bacte Notes #1 - Introduction To Bacteriology
Uploaded by
Martin ClydeOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Bacte Notes #1 - Introduction To Bacteriology
Uploaded by
Martin ClydeCopyright:
Available Formats
ADVENTIST MEDICAL CENTER COLLEGE Page |1
BACTERIOLOGY PRELIM NOTES
Definition of Terms:
Anaerobic no oxygen Culture-plant
Aerobic- with oxygen Fastidious not easily grow
Aerosol- air transmitted Gram stain test for the presence of
Agar- extract from seaweed(liquid bacteria
when heated, solid when cold) Gram positive blue/purple
Bacilli- rod-shaped Gram negative - red
Cocci- spherical Hemolytic
Colony- group from one kind Inoculation - plant
Mordant chemical that increases the
affinity of the stain
HISTORY
Robert Hooke father of cytology
Anton Van Leeuwenhoek father of microbiology
Linnaeus - nomenclature
Jenner-vaccine
Robert Koch- Germ theory
Louis Pasteur- disproved abiogenesis
Elie Mechnikoff- phagocyotosis
Watson and Crick-DNA
Prokaryotes vs. Eukaryotes
CELLULAR NON-CELLULAR
Prokaryotic Eukaryotic Virus
True Nucleus +
Cell wall +
Chromosome Haploid Diploid
DNA/RNA Either
Cell Division Binary Fission Mitosis Assemble/ Disassemble
Ribosome 70s 80s
Organelles
Size 1-5 nm 3-25nm 0.25nm
CLASSIFFICATION OF BACTERIA BASED ON MORPHOLOGY
Cocci - spherical
1. Staphylococci clusters
2. Streptococci chains
3. Pneumococci diplococci/ two
Bacilli Rods
1. Mycobacterium Tuberculosis
2. Pseudomonas
3. Salmonella typhi
4. Clostridium tetani
Spirochetes Spirals
1. Treponema
2. Leptospira
METABOLIC CHARACTERISTICS
1. Oxygen H202, O2-
ENZYMES : Catalase 2H2O2 2H2O+ O2
Peroxidase 2H2O2 2H2O+ O2
Superoxide dismutase (SOD) 2H+ + 40- 2H2O2
Martin Clyde G. Paglinawan | BACTERIOLOGY PRELIM NOTES
ADVENTIST MEDICAL CENTER COLLEGE Page |2
ORGANISM OXYGEN REQUIREMENT PATHWAY ENZYMES
Obligate Aerobe Glycolysis Catalase
Peroxidase
SOD
Facultative anaerobe Primarily Aerobic Fermentation SOD
Catalase
Microaerophilic Low Oxygen Fermentation SOD
Aerotolerant Primarily Aerobes Fermentation SOD
Obligate anaerobe Cant live without oxygen Fermentation None
2. Carbon Source
Phototrophs light
Chemotroph organic
Autotroph inorganic source
Heterotroph organic, glucose
Chemoheterotroph requires glucose, lipid, protein
Capnophilic - 10% CO2 required
Halophilic requires salt, salt-loving
NaCl (0.85%) human
1-3% - vibrio
6.5% - enterococcus
7.5% - staphylococci
3. Temperature
Psychrolic - cold, 2-10 oC, bacteria: Listeria, Yersinia
Mesophilic moderate, 20-40 oC (RT= 20-30 oC), most clinically important
Thermophilic - heat
Hyperthermophilic extreme temperature
e.g. bacteria: Bacillus stearothermophilus, Bacillus Subtilis
Other:
42oC Campylobacter
5oC Listeria
35-37oC
4. Hemolytic Pattern
Alpha partial hemolytic, green
Beta clearing of colony
Gamma no hemolysis
Alpha-prime Alpha+Beta
5. pH requirement
acidophile 3.0-6.5 pH, bacteria: Lactobacillus Lactonica lactis
alkalophile 8-10 pH, bacteria: Vibrio
neutral/slightly alkaline (7.35-7.45), optimum
GRAM STAIN
1. Gram positive blue/purple
2. Gram negative red
Exception:
Mycobacteria
Spirochetes
Mycoplasma
Martin Clyde G. Paglinawan | BACTERIOLOGY PRELIM NOTES
ADVENTIST MEDICAL CENTER COLLEGE Page |3
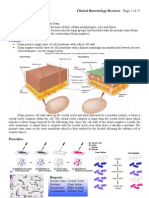
BACTERIAL STRUCTURE
1. Cell Wall (Peptidoglycan)
Techoic Acid - the affinity of the stain, G(+), crystal violet
2. Outer membrane Gram (-) rich in lipid
3. Lipopolysachharide (LPS) Gram Negative ( virulence)
Endotoxin dead
4. Periplasmic Space Gram negative, resistance,
bacteria: Lactobacilllus (Lactamase) resistance
5. Capsule protects from phagocytosis, covers antigen of bacteria,
bacteria: Neisseria meningitidis cause meningitis
6. Cell membrane energy production, cytochrome electron transport, polymoxin
7. Ribosome repair, site of protein synthesis, erythromycin
8. Plasmid nonchromosomal DNA, carries resistant gene
9. Pili/Fimbriae 2 functions:
Attachment e.g. E.Coli
Conjugation
Flagella
a. Atrichous w/out flagella
b. Monotrichous vibrio
c. Apmhitrichous both ends
d. Lopotrichous tuft of flagella
e. Petrichous surrounded by flagella
10. Endospore dormant/nonvegetation, resilient
11. Toxin
Endotoxin Gram(-), DEAD
Exotoxin gram(-)/gram(+), ALIVE, exaletanus plasmin, e.g. Botulinum flaccid
Enterotoxin holds NaCl
GROWTH CURVE the growth in bacteria is in number, NOT SIZE
1. Lag Phase adjustment
2. Log/Logarithmic/Exponential Phase ideal collection, most important, most sensitive in
antibiotic
3. Stationary/Plateau Phase Dead or Alive
4. Death Phase number of deaths exceeds number of new cells formed
BACTERIAL METABOLISM
Respiration w/ O2
Krebs Cycle
ETC (Elecrone
Glucose-CO2 and H2O
Oxidation w/ O2 Gluc-acid
Fermentation w/o O2
EMP(Embden Meyerhof Pathway)
Gluc-acid/alcohol
BACTERIAL GENETICS
Genotype genetic makeup/complete genome
Phenotype expressed(G+/G-)/observable
Plasmid extrachromosomal DNA
Transposon jumping genes w/n plasmid
Mutations change in nucleotide sequence
a. Point mutation one
b. Frameshift mutation more than one
DNA TRANSFER same objective but different mechanism
Transformation naked DNA
Transduction phages, mediated by bacteria infected by virus (bacteriophages)
Conjugation direct transfer through pili
Martin Clyde G. Paglinawan | BACTERIOLOGY PRELIM NOTES
ADVENTIST MEDICAL CENTER COLLEGE Page |4
BACTERIAL CONTROL
Sterilization all include spores, kills all forms of life
Disinfection pathogenic/flora
a. Disinfectant living, e.g. NaOCL (Hypo) 1:10
b. Antiseptics non-living, e.g. Alcohol
KILLING DEPENDS ON:
Type
Number
Chemical concentration e.g. NaOCl (1:10)
Duration of contact
Alcohol(1 min)
HIV (2 min)
HBV (10 min)
Organic matter/oil present
KILLING DEPENDS ON:
Mycolic acid acid and lipid in Mycobacterium Tuberculosis, refers to mycobacterium
Spores/dormant
Vegetative bacterial feeding stage, easy to kill
Enveloped virus unstable , note used to be exposed
Naked virus more resistant t
Chitin Fungi
LEVEL OF DISINFECTION/STERILIZATION
High sporicidal(kills the spores), tubercolocidal
Intermediate Tuberculocidal, NOT spores. e.g. Boiling
Low NOT sporicidal nor tuberculocidal. e.g. Alcohol
METHODS OF DISINFECTION AND STERILIZATION
1. Physical
Incineration dry heat, highest temp
waste disposal (870-980C)
Dry Heat Oven 160-180C / 1.5-3hrs. For glasswares
Cremation Disease control
Flaming needle/culture
Autoclave moist heat/steam under pressure. For media
15psi/121C/15-20mins
Boiling 100C/15-30mins (MTB)
Pasteurization 63C/30mins or 72C/15secs for milk
2. Filtration 100% sterility, thin membrane filters(0.22-0.45u cellulose nitrate) or cellulose
diacetate(.015-12u) for vaccines and antiobiotic
3. Chemical methods- mostly disinfectant
Formaldehyde/glutaraldehyde cold sterilant
Alcohol disinfectant (70%)
Phenol standard disinfectant/cell membrane
Zephiran (Bezalkonium Cl) use for Alcohol measurement of blood
Iodine halogen
NaOCl Hypo/Chlorox
OTHER DISINFECTANTS
Freezing
Lyophilization best for culture preservation/years
UVL pyrimidine/DNA, use in biosafety cabinet, targets DNA
H2O2 agua oxinada
Detergents cell membrane
SPECIMEN COLLECTION
Collected during acute phase/before treatment
Written order/site Sterile/non-sterile, aerobic or anaerobic
Culture/usual flora
Compared with diagnosis
Martin Clyde G. Paglinawan | BACTERIOLOGY PRELIM NOTES
ADVENTIST MEDICAL CENTER COLLEGE Page |5
SPECIMEN COLLECTION METHODS
1. Aspirate
Tissues synovial fluid, abscess, pericardial, peritoneal
Blood 1:10 / 0.025% SPS / 2-3 cultures during 24hrs (at least 10ml)
70% Alcohol + 2% Iodine (allowed to dry, not palpated)
Hemolysis (sign of bacterial growth), turbidity/BAP and CAP
CSF by doctors, never refrigerated (N and H)
BAP,CAP, Mac, India ink
2. Swab least desirable especially anaerobic bacteria
URT throat / sputum
LRT sputum less than 25 EC/greater than 10 Neutrophils
NALC (digestant) / NaOH (decontaminant) Gold standard for MTB
Wound clean, explore, obtain fresh material/quantity
Avoid drying
Requires H2O to survive
Vaginal swab (G-)
3. Urine clean perianal/catheterized
Midstream discard first few mL
Suprapubic direct to the bladder
4. Stool not Gram stained 6. Genital tracts dont expose to cold
Sterile container NOT temp
necessary Men 3-4cm swab into the
Wide-mouthed container urethra
Without urine Women no lubricants, physician
1 hour collection uses speculum
5. Throat depressed before swabbing
PRESERVATION, STORAGE AND TRANSPORT
Notes:
Neisseria Delays: Refrigerate except
Room temp (20 - 30C) CSF
Sensitive Blood
Most fastidious Swab for Neisseria
Special collection and Boric acid for urine
environment
Never use cotton for culture
Major Concerns why preserve:
Inaccurate quantitation
Death due to temp
Overgrowth
Oxygen protection for anaerobes
Loss thru dyingSafety for transport
USE OF ANTICOAGULANTS AND PRESERVATIVES
Citrate/EDTA never to be used for culture (possible contamination)
Heparin for virus
Antibiotic Removal Device (ARD) neutralizes the antibiotic
SPS (sodium polyanetholsulfonate) most common
SAS (Sodium amylsulfate)
STORAGE
Freezing (-70C) virus/ if delayed within 4 days
Ref (4C) urine ,viral blood, swabs
RT (25C) fungi
Incubator (37C) CSF, bacterial blood, agar plates
Martin Clyde G. Paglinawan | BACTERIOLOGY PRELIM NOTES
ADVENTIST MEDICAL CENTER COLLEGE Page |6
SPECIMEN LABELING AND REJECTION
Request
Patients ID/names
Source
Initial diagnosis/history,
Test requested
Suboptimal Specimens - rejected
Syringe with needles attached
Leaking
Stools with urine/barium
Non-matching request and specimen:
Non-invasive recollect
Invasive process if responsible person signs a waiver
Anaerobes from inappropriate source
Older than 2 hrs. /unpreserved / 24hrs. urine
Ref blood/CSF
Dried-up
Specimen in formalin
Non-sterile containers
QNS (Quantity Not Sufficient)
Greater than 25 EC/LPF/less than 10 neutrophils(saliva)
STAINS BACTERIAL CRAYONS
Simple One dye
Different Quellung test
Indirect/negative India ink
Gram Stain
a. 1 stain Crystal violet (stains Gram+ and Gram- blue/purple)
b. Mordant Iodine ( the affinity of the stain)
c. Decolorizer Acetone alcohol (removes CV in G- )
d. 2 stain/counter stain Safranin (stains G- red) and (G+ purple)
NOTE:
WBC and RBC pink (internal control)
Factors affecting false positive and false negative result:
a. G(+) becomes G(-) false negative
Over decolorization, old, dying
Acidic Iodine
Penicillin
b. G(-) becomes G(+) false positive
Under decolorization
Thick Smear
GRAM STAIN GENERAL RULE
All cocci are G(+) except:
Neisseria
Veillonella
Moraxella (Branhamella)
All bacilli are G(-) except:
My Mycobacteria
Corny Corynebacterium
But Bacilli
Colorful Clostridium
Lab Lactobacillus
Li Listeria
Fe Erysiphilothrix
Nocardia and actimyces
All spiral organism are reported as G(-)
Yeasts are G(+)
Martin Clyde G. Paglinawan | BACTERIOLOGY PRELIM NOTES
ADVENTIST MEDICAL CENTER COLLEGE Page |7
ACID-FAST STAIN
Differentiate AFO(Acid Fast Organism) from NAFO (Non-acid Fast Organism)
Mycolic Acid resists acid decolorization
Brightfield Fluorescence
Method Ziehl-Neelsen Kinyoun Auramine-Rhodamine
(C-A-M) (C-A-M)
1 Stain Carbol-Fuchsin (red) Carbol-Fuchsin Auramine-Rhodamine
Mordant Heat Phenol (increased
detergent)
Decolorizer 3% acid alcohol 3% acid alcohol 0.5% acid alcohol
2 Methylene Blue Malachite Green 0.5% KMnO4 quenching
Result AFO-red AFO-red AFO yellow fluorescence
NAFO - Blue NAFO - Blue NAFO No fluorescence
MICROSCOPY (OIL IMMERSION)
Magnification times an image magnified
Resolution power that two objects are really separate
Types of Microscope
Bright-field light background(0.2 um) Electron (0.001 um)
Dark-field dark background(Spiro) a. TEM (transmission) internal
Phase contrast HLA typing/living b. SEM (scanning) external
Fluorescent
UNIVERSAL PRECAUTIONS
Barrier protection gloves, masks, lab gown, puncture resistant biohazard container(color)
Color coding for waste category:
Black non-infectious dry waste
Green non-infectious wet waste
Yellow infectious and pathological waste
Yellow with black band chemical waste
Red sharp and pressurized containers
Engineering controls protects while working(BSC) from aerosols
Heat
UV
HEPA (High efficiency particulate air) removes 0.3 um particle
BIOSAFETY CABINET CLASSES
a. Class I - Open(unsterilized air circulates), exhaust air sterilized by HEPA filters, negative
b. Class II - Both air entering, circulating and exhaust is fertilized (routine)
c. Class III Entirely enclosed, highest level of safety, infectious materials are handled with gloves.
1st HEPA sterilizes supply air, 2nd HEPA for exhaust air
CULTURE MEDIA
Media contains nutrients for growth, isolation and ID, can be classified based on:
Physical State/Consistency
Solid 1.5% agar added
Semi-Solid 0.5-1% agar
Liquid no agar
Agar polysaccharide extract from seaweed/algae
Composition
Synthetic/commercial exact composition is known
Non-synthetic not exact/serum or blood/meat extract broth
Tissue culture living tissues/ immortal cells(cancer cells)
Chick embryo/eggs
A549 from lung cancer
Hela cell cervical cancer
Hep 2 cells laryngeal cancer
Martin Clyde G. Paglinawan | BACTERIOLOGY PRELIM NOTES
ADVENTIST MEDICAL CENTER COLLEGE Page |8
Dispensing/Distribution
Plated dispensed on sterile petri dish(EMB, Mac, BAP)
Preparation: Weigh Dissolve Autoclave Dispense
Tube on sterile tubes
Preparation: Weigh Dissolve Dispense Autoclave
Broth
Agar slant
Slant and butt
Butt
Use
Non-selective (CAP/BAP)
Selective inhibitory agents that does not affect the desired org. (stool)
Differential characteristics on medium(BAP)
Enriched for fastidious organism / CAP
Selective enrichment/broth media supports small numbers
Transport prevents replication
ROUTINE CULTURE MEDIA
BAP(Blood Agar Plate) fastidious/hemolysis/defibrinated blood(V factor)
CAP(Chocolate Agar Plate) Haemophilus/Neisseria/Isovitalex(X and V factors)
Thayer-Martin Agar(TMA) Modified chocolate/antibiotics added
Bacteria:
N. gonorrhoeae
N. meningitidis
Antibiotics:
Vancomycin G(+)
Colistin G(-)
Nystatin fungi (yeast)
Modified TMA added trimethoprim(proteus inhibitor)
Martin Lewis agar Neisseria / anisomycin in place of colistin
Eosin Methylene blue lactose fermentation
E and M indicators/ M inhibits G+
Mac Conkey same use w/ EMB
Bile salts and CV inhibits G+/ Neutral red (indicator)
Mannitol Salt agar(MSA) G+ isolation/ CPS not CNS
7.5% NaCl/Phenol red indicator
Phenyl Alcohol agar G+ isolation/PE inhibits G-
Selenite Broth - S and S/ Na hydrogen selenite inhibits most enterics
Xylose lysine desoxycholate - S and S/high NaCl inhibits enterics
Thioglycolate aerobes and anaerobes
ANAEROBIC CULTURE SYSTEM
Resazurin white(reduced) to pink(+)/used in PRAS
Methylene blue blue to white/pink(+)
Catalyst Palladium
Methods
Anaerobic jar 5-10% CO2
Prereduced anaerobically sterilized system (PRAS)
Anaerobic glove box
METHOD ENVIRONMENT
Aerobic Culture O2 21%
CO2 0.03%
Candle Jar O2 15%
CO2 5-10%
Anaerobic Jar O2 0%
CO2 5-10%
H2 5-10%
N2 80-90%
Martin Clyde G. Paglinawan | BACTERIOLOGY PRELIM NOTES
ADVENTIST MEDICAL CENTER COLLEGE Page |9
INOCULATION TECHNIQUES
Streaking accurate colony count. 2 purposes:
Quantitative
Isolated Colony
Semi Quantitative dilution streaks: yields isolates from pure colony
Key Characteristics presumptive Dx, reduces cost, QC on automation
Colony size (staph,strep,fungi)
Pigments
Staph (gold) Serratia (red)
Pseudomonas (green-yellow) Salmonella (Dark/Black)
E. coli ( ) TSI (yellow)
Shape/surface appearance (proteus,Kleibsiella)
Hemolysis
Odor pseudo (grapelike)
ANTIMICROBIAL THERAPY
Antibiotic chemical
Antimicrobial therapy use to treat Disease
(-cidal) kill
(- static) inhibits growth
Synergistic (1+1=3)
Antagonism ( 2 + 1 = 1)
Additive (1+1=2)
Indifference (A + B =A)
Broad spectrum Both G(+)/G(-) ; e.g. Tetracyclin
Narrow Spectrum either G (-) / G (+)
S Sensitive I Intermediate R Resistant
BACTERIAL ACTIVIES ON:
1. CELL WALL
B lactam antibiotics binds with transpeptidase (peptidoglycan interrupted)
Penicillin
Cephalosporin
Monobactams
B lactamase combined w/ B lactam drugs
Clavulanic acid
Sulbactam
Tazobactam
Other antibiotics
Vancomycin MRSA (methicillin-resistant Staphylococcus aureus)
Bacitracin S. pyogenes
Cycloserine Clostridia
2. CELL MEMBRANE
Polymyxin active against G(-) bacteria (phospholipids)
Bacitracin active against G(+) bacteria
3. PROTEIN SYNTHESIS interference in bacterial protein synthesis at 30s
Aminoglycoside G(-) and Staph, 30s(pseudomonas)
Tetracycline 30s (Broad spectrum)
Macrolides 50s
Chloramphenicol 50s (aplastic anemia)
4. METABOLITES prevents the synthesis of folic acid
Sulfonamides primarily treatment of UTI
Trimethoprim treatment of Chronic UTI
5. NUCLEIC ACID inhibition of bacterial DNA and RNA
Rifampin
Quinolones
Metronidazole
Naldixic acid
Martin Clyde G. Paglinawan | BACTERIOLOGY PRELIM NOTES
ADVENTIST MEDICAL CENTER COLLEGE P a g e | 10
GRAM POSITIVE COCCI (MICROCOCCACEAE)
TEST STAPHYLOCOCCUS MICROCOCCUS
Coagulase V Neg
Oxidation-Fermentation F O
Bacitracin Resistant Sensitive
Lyostaphin Sensitive Resistant
Modified Oxidation - +
CLINICALLY SIGNIFICANT SPECIES:
STAPHYLOCOCCI Gram (+) cocci Catalase (+)
S. Aureus - golden yellow colony, G+ in clusters
Gram(+) cocci Catalase(+) Coagulase(+)
Virulence Factors:
Enterotoxin A-E food poisoning
Enterotoxin F/Exotoxin C/TSST-1 Toxic shock syndrome
Exfoliatin SSS(skin scalded syndrome)
Protein A antiphagocytic/binds Fc portion
Leukocidin Panton-Valentine factor
Enzymes catalase, coagulase, DNAse, hyaluronidase, lipase, B-lactamase
S. Epidermidis nosocomial UTI(most common)/slime adheres to prosthetic heart valves
Gram(+) cocci Coagulase(-) Novobiocin (S)
S. Saprophyticus UTI among sexually active women/adheres to urogenital tracts low numbers
are significant
Gram(+) cocci Coagulase(-) Novobiocin (R)
Micrococcus
Gram (+) cocci Catalase (+) Modified Oxidation (+)
PRESUMPTIVE AND DIAGNOSTIC TESTS Staphylococci
Microscopic exam Gram(+) cocci in clusters
Culture Golden yellow/white(MSA 7.5% NaCl)
Catalase 3% H2O2(reagent) /+ gas(staph)/bubbles
Modified oxidase (microdase) (+ in 30sec)
Coagulase clot formation
Slide screening/bound coagulase (Clumping Factor)
NSS + org
Tube confirm/free or unbound (Coagulation Factor)
rabbits plasma/human plasma (pt and ptt normal) + 37C for 4hrs(clot)/
BAP avoid touching the agar
Latex coagulation CF and protein A
5 ug Novobiocin Resistance/Zone of Inhibition = 16mm
Antibiotic Penicillin(w/o B-lactamase)
Methicillin PRSA
Vancomycin MRSA
Martin Clyde G. Paglinawan | BACTERIOLOGY PRELIM NOTES
ADVENTIST MEDICAL CENTER COLLEGE P a g e | 11
STREPTOCOCCI
BETA-HEMOLYTIC BACTERIA (LANCEFIELD GROUPS) carbohydrate composition of bacterial antigens
found in their cell wall
Group A
S. Pyogenes
Disease: Tonsilitis Rheumatic Fever Acute Glomerulonephritis (AGN)
Test:
CAMP (-) absence of arrowhead; reagent Cyclic adenosine monophosphate
PYR (+) red color result; reagent P-dimethylamino-cinnamaldehyde
Taxo A (Bacitracin Test) Sensitive (no zone of inhibition)
Hippurate Hydrolysis no color change; reagent Sodium Hippurate
Group B
S. Agalactiae
Disease:
Neonatal Meningitis
Otitis Media
Test:
CAMP (+) arrowhead result; reagent - Cyclic adenosine monophosphate
Hippurate Hydrolysis (+) purple/violet result; reagent Sodium Hippurate
ALPHA-HEMOLYTIC BACTERIA (NON-LANCEFIELD GROUPS)
S. Pneumoniae / Pneumococci (diplococci)
Lancet-shaped
Disease:
Pneumonia
Acute Bacterial Meningitis
Test:
Bile Solubility (+) clearing result; reagent 10% Desoxycholate(BAP) and
2% Desoxycholate(Tube)
Taxo P (Optochin Test) sensitive (Zone of Inhibition = 14mm)
Quellung (+) swelling result; reagent antibody
India Ink
Viridans
Test:
Bile Solubility (-) no clearing of turbidity 10% Desoxycholate(BAP) and
2% Desoxycholate(Tube)
Quellung (-) no swelling
Taxo P (Optochin Test) resistant (Zone of Inhibition = 14mm)
S. Sanguis
o Disease: Subacute endocarditis
S. Mutans
o Disease: Dental Cavities
GAMMA-HEMOLYTIC BACTERIA
Group D
Enterococcus: E. Faecalis
Test:
Bile Esculin (+) Black color result; reagent Oxgall (Bile Salts)
6.5% NaCl (+) turbidity result / yellow color
PYR (+) Red color result; reagent P-dimethylamino-cinnamaldehyde
Non-enterococcus: S. Bovis
Test:
Bile Esculin (+) Black color result; reagent Oxgall (Bile Salts)
6.5% NaCl (-) clear result/ no growth / no color change
PYR (-) yellow/orange color result ; reagent P-dimethylamino-cinnamaldehyde
Martin Clyde G. Paglinawan | BACTERIOLOGY PRELIM NOTES
ADVENTIST MEDICAL CENTER COLLEGE P a g e | 12
Note:
Nutrionally Variant Stretococci (NVS)
Abiotrophia without life, needed vitamin B6 to grow
BACTERIAL TESTS
1. Gram Staining differentiate bacteria into two large groups
Reagent:
1o stain Crystal Violet
Mordant Iodine
Decolorizer acetone alcohol
Counter stain Safranin
Result:
Positive purple
Negative red
2. Catalase Test differentiate Staphylococcus from Streptococcus
Reagent
H202 Hydrogen Peroxide
Result
Positive bubbling reaction; bacteria Staphyloccus / Micrococcus
Negative no bubbling reaction; bacteria Streptococcus
3. Modified Oxidation differentiate Staphylococcus from Micrococcus
Result:
Positive Micrococcus
Negative Stapylococcus
4. Coagulase Test differentiate S. Aureus from Catalase Negative Staphlylococcus
Reagent:
Rabbit plasma/Human plasma
Slide Coagulase Test clumping factor
Result:
Positive clumping cocci; bacteria S. Aureus
Negative no clumping; bacteria S. Epidermidis / S. Saprophyticus
Tube Coagulase Test coagulation factor
Result:
Positive coagulate; bacteria S. Aureus
Negative no coagulation; bacteria S. Epidermidis / S. Saprophyticus
5. Novobiocin differentiate S. Epidermidis from S. Saprophyticus
Reagent:
Novobiocin (Zone of Inhibition = 16mm)
Result:
Sensitive S. Epidermidis
Resistant S. Saprophyticus
6. Hemolysis used to classify streptococci species
Reagent:
Blood Agar Plate
Result:
Alpha partial hemolysis / green; bacteria S.Pneumoniae and S. Viridans(2)
Beta complete hemolysis / yellow ; bacteria S. Pyogenes and S.Agalactiae and
other Lancefield Groups
Gamma no hemolysis/unchanged; bacteria Group D Streptococcus: E. Faecalis
and S. Bovis
7. Bacitracin(TAXO A) differentiate S. Pyogenes and Group B Streptoccus: S. Agalactiae
Reagent:
Bacitracin (No Zone of Inhibition)
Result
Sensitive S. Pyogenes
Resistant S. Agalactiae
Martin Clyde G. Paglinawan | BACTERIOLOGY PRELIM NOTES
ADVENTIST MEDICAL CENTER COLLEGE P a g e | 13
8. CAMP Test differentiate Group B Streptococcus: S. Agalactiae from other Lancefield group
Named after 3 researchers who discovered ( Christie, Atkins, Munch-Petersen )
Reagent:
Cyclic adenosine monophosphate
Result:
Positive arrowhead; bacteria Group B: S. Agalactiae
Negative absence of arrow head; bacteria other Lancefield groups
9. Bile Solubility Test identify S. Pneumoniae from bile-insoluble Streptococci
Reagent:
10% Desoxycholate (BAP)
2% Desoxycholate (Tube)
Result:
Positive clearing of turbidity; bacteria S. Pneumoniae
Negative no clearing of turbidity; bacteria bile-insoluble Streptococi
10. Optochin Test (TAXO P) - identify S. Pneumoniae from Optochin-resistant Streptococci
Reagent:
Optochin (Zone of Inhibition 14mm)
Result:
Sensitive S. Pneumoniae
Resistant Optochin-resistant Streptococci
11. Bile Esculin Test identify Group D Streptococcus from other Streptococci
Reagent:
Oxgall (bile salts)
Result:
Positive black color; bacteria Enterococcus: E. Faecalis/Nonenterococcus: S. Bovis
Negative no black color form; bacteria other Streptococci
12. 6.5% NaCl Test - differentiate Enterococcus from Non-Enter.
Reagent:
Sodium Chloride
Result:
Positive turbidity / yellow color; bacteria Enterococcus: E. Faecalis
Negative no turbidity / no color change; bacteria Non-enterococcus: S. Bovis
13. PYR (Pyrrolidonyl Arylamidase) Test presumptive identification of group A Beta-Hemolytic
Streptococci and differentiate Enterococcus: E. Faecalis and Non-Enterococcus: S. Bovis
Reagent:
P-dimethylamino-cinnamaldehyde
Result:
Positive color red; bacteria S. Pyogenes and Enterococcus: E. Faecalis
Negative yellow/orange color; bacteria Non-Enterococcus: S. Bovis
14. Hippurate Hydrolysis Test presumptive identification Group B streptococci: S. Agalactiae
Reagent:
Sodium Hippurate
Ninhydrin Reagent
Result:
Positive purple/violet color; bacteria S. Agalactiae
Negative no color change; bacteria S. Pyogenes
END
Prelim Exam Type of Test
Multiple Choice 50%
Identification 30%
Matching type/ True or False 10 %
Book 10%
Martin Clyde G. Paglinawan | BACTERIOLOGY PRELIM NOTES
ADVENTIST MEDICAL CENTER COLLEGE P a g e | 14
Martin Clyde G. Paglinawan | BACTERIOLOGY PRELIM NOTES
You might also like
- 1-Cell Organelles WS 2016 KEYDocument2 pages1-Cell Organelles WS 2016 KEYElvin Hoyo-a Logroño100% (2)
- Stages of Fetal Development FinalDocument43 pagesStages of Fetal Development Finalsanthiyasandy100% (6)
- Mycology and VirologyDocument18 pagesMycology and VirologyDreyden Halo100% (1)
- Reviewer - Immunoserology - Part 1Document12 pagesReviewer - Immunoserology - Part 1Joshua Trinidad0% (1)
- Bacteriology PDFDocument49 pagesBacteriology PDFPearl Medina100% (2)
- Parasitology SummaryDocument2 pagesParasitology SummarythescarletpimpernelsNo ratings yet
- Anion Gap CalculationDocument13 pagesAnion Gap CalculationDams ZainalNo ratings yet
- Microbiology Boards Lecture 1Document48 pagesMicrobiology Boards Lecture 1Fait Hee100% (3)
- Bacterial Identification Methods SummaryDocument12 pagesBacterial Identification Methods SummaryLarnie Alejandre100% (1)
- Upper and Lower Limb Clinical Notes (Snell)Document12 pagesUpper and Lower Limb Clinical Notes (Snell)Martin Clyde100% (1)
- (Biophysical Techniques Series) Iain D. Campbell, Raymond A. Dwek-Biological Spectroscopy - Benjamin-Cummings Publishing Company (1984)Document192 pages(Biophysical Techniques Series) Iain D. Campbell, Raymond A. Dwek-Biological Spectroscopy - Benjamin-Cummings Publishing Company (1984)BrunoRamosdeLima100% (1)
- Summary of Key Microbiology TestsDocument45 pagesSummary of Key Microbiology TestsAtiya HajjajNo ratings yet
- Clinical Bacteriology ReviewerDocument17 pagesClinical Bacteriology Reviewernkivc100% (5)
- ParasitologyDocument27 pagesParasitologyDreyden HaloNo ratings yet
- Bacteriology HandoutsDocument30 pagesBacteriology HandoutsMarco Tolentino100% (8)
- HistopathDocument23 pagesHistopathElla SalesNo ratings yet
- MycologyDocument26 pagesMycologySkandi43No ratings yet
- BacteriologyDocument13 pagesBacteriologyGlydenne Glaire Poncardas Gayam33% (3)
- Bacteriology LectureDocument38 pagesBacteriology LectureAisle Malibiran Paler100% (1)
- Virology TableDocument10 pagesVirology TablekevinNo ratings yet
- MYCO-VIRO LEC Practical Exam ReviewerDocument5 pagesMYCO-VIRO LEC Practical Exam ReviewerJoseph SabidoNo ratings yet
- Parasitology Review Notes For Medical Technologists: Leishmania SPP)Document39 pagesParasitology Review Notes For Medical Technologists: Leishmania SPP)Kat Jornadal100% (2)
- IMS - Immunomodulation & ImmunodeficienciesDocument3 pagesIMS - Immunomodulation & ImmunodeficienciesJeanne RodiñoNo ratings yet
- Hematology Ii Lectures Introduction To HemostasisDocument28 pagesHematology Ii Lectures Introduction To HemostasisJoshua Trinidad100% (1)
- Parasitology TableDocument4 pagesParasitology TableJae MinionNo ratings yet
- Agents of Mycoses Identification and CharacteristicsDocument44 pagesAgents of Mycoses Identification and CharacteristicsRia AlcantaraNo ratings yet
- Blood Banking Course BookDocument2 pagesBlood Banking Course BookShukr Wesman BlbasNo ratings yet
- (Microbio) Staphyloccocus and Streptococcus-Dr. Salandanan (BHND)Document16 pages(Microbio) Staphyloccocus and Streptococcus-Dr. Salandanan (BHND)Lee Delos Santos100% (1)
- Staphylococci: Streptococcus PyogenesDocument20 pagesStaphylococci: Streptococcus PyogenesPharmacy2015100% (2)
- Parasitology-Lec 3 Nematodes 2Document6 pagesParasitology-Lec 3 Nematodes 2api-3743217100% (4)
- Gram Positive Cocci Sem 1 1Document45 pagesGram Positive Cocci Sem 1 1Charmaine Corpuz Granil100% (1)
- Microbio Lec 1 - Bacterial Morphology and Ultra StructureDocument8 pagesMicrobio Lec 1 - Bacterial Morphology and Ultra Structureapi-3743217100% (3)
- Molecular Biology and Diagnostic Intro To CytogeneticsDocument6 pagesMolecular Biology and Diagnostic Intro To Cytogeneticselijah montefalcoNo ratings yet
- Viral Basics and Replication CyclesDocument21 pagesViral Basics and Replication CyclesfrabziNo ratings yet
- Bacteriology SummaryDocument35 pagesBacteriology SummarykevinNo ratings yet
- Clinical Chemistry KeyNotes For Board ExaminationDocument12 pagesClinical Chemistry KeyNotes For Board ExaminationPrincess Alen Aguilar100% (1)
- 3 SEMR421 Bacteriology Part 3Document14 pages3 SEMR421 Bacteriology Part 3Micah Daniel TapiaNo ratings yet
- Protozoa Summary TableDocument1 pageProtozoa Summary TablejustNo ratings yet
- Bacteriology Study SheetDocument50 pagesBacteriology Study Sheetvishal_life27100% (5)
- MICROBIOLOGY MEDIADocument3 pagesMICROBIOLOGY MEDIAAisle Malibiran PalerNo ratings yet
- Parasitology-Lec 5 TrematodesDocument5 pagesParasitology-Lec 5 Trematodesapi-3743217100% (2)
- Microbiology ReviewDocument22 pagesMicrobiology ReviewCassie Von Peenq100% (1)
- IMS - Intro To Immunology and SerologyDocument3 pagesIMS - Intro To Immunology and SerologyJeanne RodiñoNo ratings yet
- HistopathDocument37 pagesHistopathFait HeeNo ratings yet
- Culture Medium Components and PreparationDocument5 pagesCulture Medium Components and PreparationGlydenne Glaire Poncardas GayamNo ratings yet
- Medical Parasite TableDocument3 pagesMedical Parasite Tablesidman47100% (2)
- MUST To KNOW in ParasitologyDocument22 pagesMUST To KNOW in ParasitologyTristan Jay CalabiaNo ratings yet
- Intestinal Nematodes Maricelle ManlutacDocument64 pagesIntestinal Nematodes Maricelle ManlutacGlanela ManalotoNo ratings yet
- Compre HistopatDocument21 pagesCompre HistopatMark FuerteNo ratings yet
- MUST To KNOW in BacteriologyDocument34 pagesMUST To KNOW in BacteriologyRona Salando91% (11)
- Clinical Microscopy ExamDocument3 pagesClinical Microscopy ExamKarla GiorlaNo ratings yet
- Mycology and VirologyDocument8 pagesMycology and VirologyMaybelle Acap PatnubayNo ratings yet
- BacteriologyDocument1 pageBacteriologyCaryn RobertsonNo ratings yet
- Histopathologic and Cytologic Techniques Lecture: General Pathology: An IntroductionDocument11 pagesHistopathologic and Cytologic Techniques Lecture: General Pathology: An IntroductionTheresa BergonioNo ratings yet
- TrematodesDocument9 pagesTrematodesJoseph PerezNo ratings yet
- Must To Know in Immunology and Serology ImmunologyDocument19 pagesMust To Know in Immunology and Serology ImmunologyCath PortezNo ratings yet
- Gram Negative Cocci (Lecture Notes)Document5 pagesGram Negative Cocci (Lecture Notes)Dayledaniel Sorveto100% (1)
- MID Bacteria Charts JkuoDocument17 pagesMID Bacteria Charts Jkuotsukino143100% (2)
- Clinical Chemistry NotesDocument24 pagesClinical Chemistry Notesclower112100% (3)
- Immunology Serology ReviewDocument211 pagesImmunology Serology ReviewRachel Marie M. Gania100% (1)
- Agglutination, Complement, Neutralization, and Inhibition: Methods in Immunology and Immunochemistry, Vol. 4From EverandAgglutination, Complement, Neutralization, and Inhibition: Methods in Immunology and Immunochemistry, Vol. 4No ratings yet
- MICROBIOLOGYDocument7 pagesMICROBIOLOGYjiangNo ratings yet
- Klubsybear Additional Recalls: Hematology A.karyolysisDocument2 pagesKlubsybear Additional Recalls: Hematology A.karyolysisMartin ClydeNo ratings yet
- Hip FracturesDocument6 pagesHip FracturesMartin ClydeNo ratings yet
- Source: 20 Harrison's Principles of Internal Medicine: Nephrolithiasis/Kidney Stone DiseaseDocument8 pagesSource: 20 Harrison's Principles of Internal Medicine: Nephrolithiasis/Kidney Stone DiseaseMartin ClydeNo ratings yet
- Dyspnea Causes and TypesDocument3 pagesDyspnea Causes and TypesMartin ClydeNo ratings yet
- Anatomy Quick NotesDocument2 pagesAnatomy Quick NotesMartin ClydeNo ratings yet
- Impaired fetal development linked to maternal nutritionDocument11 pagesImpaired fetal development linked to maternal nutritionMartin ClydeNo ratings yet
- Hip FracturesDocument6 pagesHip FracturesMartin ClydeNo ratings yet
- Anatomy ListDocument9 pagesAnatomy ListMartin ClydeNo ratings yet
- AbortionDocument2 pagesAbortionMartin ClydeNo ratings yet
- GoutDocument3 pagesGoutMartin ClydeNo ratings yet
- 2015 Pocket Guide CDC ITSDocument24 pages2015 Pocket Guide CDC ITSfelix camposNo ratings yet
- Forensics Chapter 7Document17 pagesForensics Chapter 7Martin ClydeNo ratings yet
- Observing Microorganisms Through A Microscope: Lectures Prepared by Christine L. CaseDocument51 pagesObserving Microorganisms Through A Microscope: Lectures Prepared by Christine L. CaseMartin ClydeNo ratings yet
- Parasitology Diagnostic Methods: Stool, Blood, and Tissue Specimen CollectionDocument12 pagesParasitology Diagnostic Methods: Stool, Blood, and Tissue Specimen CollectionMartin ClydeNo ratings yet
- Nej MP 1706474Document3 pagesNej MP 1706474Pablo IgnacioNo ratings yet
- Trypanosoma cruzi causes Chagas diseaseDocument11 pagesTrypanosoma cruzi causes Chagas diseaseMartin ClydeNo ratings yet
- Microscopy ReviewDocument30 pagesMicroscopy ReviewMartin ClydeNo ratings yet
- Parvo BacteriaDocument4 pagesParvo BacteriaMartin ClydeNo ratings yet
- Prelim ExamDocument2 pagesPrelim ExamMartin ClydeNo ratings yet
- Analytical Equipment: High AccuracyDocument6 pagesAnalytical Equipment: High AccuracyMartin ClydeNo ratings yet
- INTRO TO MT Quiz 1Document1 pageINTRO TO MT Quiz 1Martin ClydeNo ratings yet
- Midterm Grade (Lab)Document3 pagesMidterm Grade (Lab)Martin ClydeNo ratings yet
- Prelim Lab Exam Answer SheetDocument2 pagesPrelim Lab Exam Answer SheetMartin ClydeNo ratings yet
- Semi Final (Lab)Document2 pagesSemi Final (Lab)Martin ClydeNo ratings yet
- Prelim Grade (Lecture)Document3 pagesPrelim Grade (Lecture)Martin ClydeNo ratings yet
- Hot Air Oven Dso-D / DsDocument6 pagesHot Air Oven Dso-D / DsMartin ClydeNo ratings yet
- Prelim Grade (Lab)Document3 pagesPrelim Grade (Lab)Martin ClydeNo ratings yet
- Midterm Grade (Lecture)Document3 pagesMidterm Grade (Lecture)Martin ClydeNo ratings yet
- Mitosis PowerpointDocument31 pagesMitosis PowerpointLeenfranzen MagadiaNo ratings yet
- CH 16 WorkbookDocument10 pagesCH 16 Workbookapi-237586441No ratings yet
- Typhoid Fever - An Overview Good Hygiene Is The Key To Prevent Typhoid FeverDocument8 pagesTyphoid Fever - An Overview Good Hygiene Is The Key To Prevent Typhoid FeverSyarifahNo ratings yet
- r148912351 Yohanys Torres CUR148912351Document1 pager148912351 Yohanys Torres CUR148912351Yohanys TorresNo ratings yet
- Gerhard Viljoen: Top SkillsDocument22 pagesGerhard Viljoen: Top SkillsAnonymous rvCeDVNo ratings yet
- Protein Gel Electrophoresis Tips and Troubleshooting GuideDocument16 pagesProtein Gel Electrophoresis Tips and Troubleshooting Guidedrd@tiacnetNo ratings yet
- Biological Classification Class 11 Notes BiologyDocument6 pagesBiological Classification Class 11 Notes BiologyVyjayanthiNo ratings yet
- Microbiology Sheet MCQ - Part 1Document12 pagesMicrobiology Sheet MCQ - Part 1MahmOod Gh100% (3)
- Heredity and Variation.Document6 pagesHeredity and Variation.AnweNo ratings yet
- Status of Biological Diversity in Malaysia and Threat Assessment of Plant Species in MalaysiaDocument298 pagesStatus of Biological Diversity in Malaysia and Threat Assessment of Plant Species in MalaysiaCR MamRe Garingging100% (1)
- Grade 11 - Mango Vaccination InformationDocument2 pagesGrade 11 - Mango Vaccination InformationKENNEDY VAGAYNo ratings yet
- BLOOD PRODUCTS COLLECTION & STORAGEDocument14 pagesBLOOD PRODUCTS COLLECTION & STORAGESathish SizzyNo ratings yet
- Differences between Sexual and Asexual ReproductionDocument12 pagesDifferences between Sexual and Asexual ReproductionrosalynNo ratings yet
- How Living Things ReproduceDocument44 pagesHow Living Things ReproduceChristopher Agustin Tambogon LptNo ratings yet
- Activity No. 3: Structure of A Cell and MitosisDocument9 pagesActivity No. 3: Structure of A Cell and MitosisEricka GenoveNo ratings yet
- Biotechnology and Its ApplicationsDocument2 pagesBiotechnology and Its ApplicationsEunice BasarioNo ratings yet
- ENDOSIGN Review v0 EdmvDocument33 pagesENDOSIGN Review v0 EdmvMavi Camarasa SabaterNo ratings yet
- Ammonium Sulfate Saturation TableDocument4 pagesAmmonium Sulfate Saturation Tableritesh kumarNo ratings yet
- STS Module 8 Gene TheraphyDocument7 pagesSTS Module 8 Gene Theraphyjevieconsultaaquino2003No ratings yet
- Integrated modeling system for structural biologyDocument10 pagesIntegrated modeling system for structural biologyAhmed MashalyNo ratings yet
- Bai Tap Ap Dung Unit 10 Lop 12Document8 pagesBai Tap Ap Dung Unit 10 Lop 12Mai PhuongNo ratings yet
- Chapter 7 Bio Test Study Guide BDocument4 pagesChapter 7 Bio Test Study Guide BRachel FrankenfieldNo ratings yet
- IGCSE Biology Revision Notes - Kingdoms, ClassificationDocument4 pagesIGCSE Biology Revision Notes - Kingdoms, ClassificationClara ToNo ratings yet
- The Impact of IPR on Biodiversity and Genetic ErosionDocument9 pagesThe Impact of IPR on Biodiversity and Genetic ErosionMuHAMMAD Ziya ul haqq QuraishyNo ratings yet
- Four Principles of Rational Nutrition.Document6 pagesFour Principles of Rational Nutrition.machohinge3570No ratings yet
- Natural Selection Quiz Review Guide Answer KeyDocument1 pageNatural Selection Quiz Review Guide Answer KeyHelen SagaNo ratings yet
- DNA Extraction and Polymerase Chain ReactionDocument2 pagesDNA Extraction and Polymerase Chain ReactionDudungNo ratings yet